
Introduction
Employers invest heavily in employee benefits—averaging $13.79 per hour worked, or nearly 30% of total compensation. Yet despite this substantial investment, a troubling gap persists: 51% of employees say they still don't fully understand their health policies. This awareness deficit isn't just a minor inconvenience—26% of Americans have received higher-than-expected medical bills because they didn't understand their coverage.
The problem isn't the benefits themselves—it's the communication. Complex jargon, single-channel delivery, and annual-only messaging leave employees confused and benefits underutilized.
This article delivers 25 actionable tips, organized into five strategic themes, to help HR and communications leaders build a benefits communication strategy that actually reaches every employee and maximizes your investment.
TLDR
- Write in plain, jargon-free language targeting a sixth-grade reading level
- Deliver messages through multiple channels: mobile apps, SMS, email, and digital signage
- Communicate year-round, not just during open enrollment
- Personalize content by employee segment, life stage, and communication preference
- Track performance metrics and use data to continuously improve
Craft Benefits Messages Employees Actually Understand (Tips 1–5)
Clarity is the foundation of effective benefits communication. No multi-channel strategy will save a confusing message—what you say matters as much as how you send it.
Tip 1: Write at a Fifth-Grade Reading Level
HR professionals live and breathe benefits terminology, making it easy to forget how confusing this language sounds to employees. The American Medical Association and National Institutes of Health recommend health materials be written at a sixth-to-eighth-grade reading level, yet most insurance documents score at an 11th-to-14th-grade level.
Action steps:
- Test your content with Hemingway App or Grammarly to check reading level
- Target a Flesch-Kincaid score of 60 or higher
- Replace complex sentences with shorter, direct statements
- Read your content aloud—if you stumble, employees will too
Tip 2: Lead With "What's in It for Me?"
Employees tune out abstract plan descriptions but pay attention when you connect benefits directly to their real-life situations. Instead of "access to telehealth services," frame it as "a doctor available at 2am when your child has a fever."
This approach transforms generic information into personal value. List features only after you've shown how each one solves a real problem your employees face.
Tip 3: Swap Jargon for Real-World Scenarios
Only 32% of employees with High-Deductible Health Plans can correctly answer basic true/false questions about Health Savings Accounts — and 49% of Americans incorrectly believe copays count toward deductibles.
Replace industry terms with plain explanations:
| Instead of... | Say... |
|---|---|
| "Co-insurance is the percentage you pay after meeting your deductible" | "After you've paid $1,500 this year, you'll pay 20% of the bill — we cover the other 80%" |
| "Your HSA is a tax-advantaged account" | "This account lets you set aside pre-tax dollars to pay for doctor visits and prescriptions" |
| "In-network providers are covered at a higher benefit level" | "Seeing a doctor in our network costs you less — sometimes half the price of an out-of-network visit" |
Use specific dollar amounts and real scenarios employees recognize, like routine doctor visits or prescription refills.
Tip 4: Go Visual — Use Infographics, Short Videos, and Icons
Visual content moves the needle on comprehension. Research shows 88.7% of participants who viewed infographics correctly answered comprehension questions, versus 66.7% who read text-only content — a 22-point gap that directly affects enrollment decisions.
Effective visual formats:
- 60-second explainer videos showing how to use specific benefits
- Comparison graphics illustrating plan differences side-by-side
- Branded icon sets for quick benefit identification
- Process infographics breaking down enrollment steps
Even a simple side-by-side chart comparing plan deductibles and out-of-pocket maximums can cut inbound HR questions during open enrollment.

Tip 5: Keep Every Communication Bite-Sized and Scannable
Apply the "one benefit, one message" principle. Rather than covering everything in one long email, send focused, shorter communications with clear headlines, bullet points, and a single call to action.
Structure each message with:
- A descriptive subject line that states the benefit
- 2-3 short paragraphs maximum
- Bulleted key points for scanning
- One clear action step
- A link to more detailed information
When employees know exactly what to do next, open rates climb and enrollment confusion drops.
Meet Employees Where They Are: Multi-Channel Delivery (Tips 6–10)
The best benefits message is worthless if it doesn't reach the right employee at the right time in the right place. A multi-channel approach is essential for diverse workforces.
Tip 6: Build a Multi-Channel Distribution Strategy
Different employees respond to different channels. Data cited by MyBentek shows that organizations using automated, multi-channel communications achieve 28% higher enrollment participation rates than those relying on traditional methods.
Effective benefits communication requires intentional channel mapping:
- Email: Detailed information for desk-based employees
- SMS: Time-sensitive reminders and deadlines
- Mobile apps: On-demand access to plan details
- Intranet: Centralized resource hub
- Digital signage: High-visibility announcements in common areas
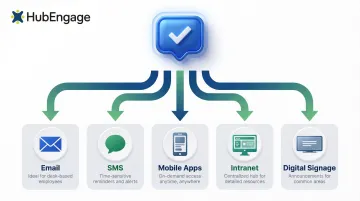
Don't blast one format to everyone—map channels to employee work patterns and preferences.
Tip 7: Prioritize Mobile-First Access for Frontline and Deskless Workers
Frontline workers in healthcare, manufacturing, hospitality, and retail rarely sit at a desk, making email alone an ineffective channel. These employees need benefits information delivered directly to their phones through mobile apps and SMS.
Platforms like HubEngage are designed specifically for this challenge, with mobile apps and auto-formatting that push benefits content to employees wherever they are, without requiring a company email address. This ensures your warehouse workers, nurses, hotel staff, and retail associates receive the same timely information as corporate employees.
Tip 8: Use Digital Signage in Break Rooms and Common Areas
Digital displays are high-visibility channels for announcing open enrollment deadlines, spotlighting specific benefits, and sharing reminders in the physical spaces where employees naturally gather.
Place screens strategically in:
- Break rooms and cafeterias
- Manufacturing floor entrances
- Nursing stations
- Retail back-of-house areas
- Lobby and reception areas
Rotate content regularly to maintain attention and highlight different benefits throughout the year.
Tip 9: Leverage SMS and Push Notifications for Urgent, Time-Sensitive Messages
SMS dramatically outperforms email for immediate engagement. SMS achieves a 98% open rate and 22.2% click-through rate, compared to email's 43% open rate and 2.5% click-through rate.
Use SMS for:
- Open enrollment deadline reminders
- "Last chance to enroll" alerts
- FSA/HSA spending deadline notifications
- New benefit announcement alerts
- Life event change reminders
Keep messages brief, include a clear action, and provide a link to additional information.
Tip 10: Create a Centralized Benefits Hub Employees Can Return To Anytime
Once employees know where to go, they stop calling HR for answers. Build a persistent resource (an intranet page, mobile app, or digital portal) where employees can always find plan details, FAQs, contacts, and enrollment links. Self-service access reduces help desk volume year-round.
Your benefits hub should include:
- Current plan summaries and comparison charts
- Enrollment guides and video tutorials
- Provider directories and contact information
- Frequently asked questions
- Claims submission instructions
- Wellness program details
Make the hub searchable and mobile-responsive so employees can access it from any device.
Build a Year-Round Communication Calendar (Tips 11–15)
Most employees hear about their benefits once a year — and forget most of it by February. A year-round communication calendar changes that by keeping benefits relevant, visible, and actually used.
Tip 11: Map Out a 12-Month Benefits Communication Calendar
Build a full-year editorial calendar with quarterly themes, seasonal spotlights, and planned touchpoints that prevent communication blackouts.
Sample calendar structure:
- Q1: New year wellness kickoff, HSA/FSA maximums, preventive care reminders
- Q2: Mental health awareness, financial wellness education
- Q3: Flu shot campaigns, open enrollment preparation
- Q4: FSA spend-down reminders, year-end wellness challenges
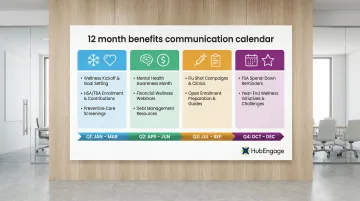
Schedule at least one benefits touchpoint per month, increasing frequency during open enrollment periods.
Tip 12: Trigger Communications Around Employee Life Events
Automated, event-triggered messaging delivers relevant information exactly when employees need it. Set up sequences for:
- New hire benefits orientation (day 1, week 1, week 4)
- Marriage or family addition reminders about coverage changes
- Qualifying life event notifications
- EAP resource reminders when employees go on leave
- Pre-retirement planning for employees approaching eligibility
When a message arrives right after a life change, employees act on it — enrollment rates for triggered campaigns consistently outperform bulk communications.
Tip 13: Start Open Enrollment Communications Early and Build Momentum
Despite recommendations to begin communications 1-2 months before enrollment, 57% of employers only communicate in the weeks leading up to the period.
Effective timeline:
- 4-6 weeks before: Teaser phase announcing dates and what's new
- 2-4 weeks before: Education phase explaining plan options and changes
- During enrollment: Action phase with reminders, deadlines, and support resources
- After enrollment: Confirmation and "what's next" guidance
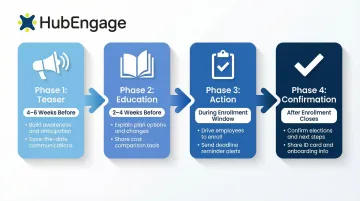
This phased approach builds awareness gradually rather than overwhelming employees with a single blast.
Tip 14: Use Seasonal Moments to Spotlight Relevant Benefits
Tie benefits communications to what employees are naturally thinking about:
- January: New year health goals, HSA/FSA maximums
- May: Mental Health Awareness Month → highlight EAP
- October: Financial Wellness Month → promote 401(k) matching
- November: Flu season → telemedicine and preventive care
- December: FSA spend-down reminders, holiday stress resources
Benefits tied to a current moment don't just get read — they get used.
Tip 15: Don't Go Silent After Open Enrollment Closes
Employees who enroll but never hear about their benefits again are unlikely to use them effectively. Schedule monthly or quarterly touchpoints that:
- Highlight a single benefit in depth
- Share utilization tips and success stories
- Celebrate wellness milestones
- Remind employees of underutilized benefits
Teams that maintain this cadence typically see higher benefit utilization rates — which directly supports both employee wellbeing and your ROI on the benefits package itself.
Personalize Benefits Communications for Your Workforce (Tips 16–20)
One-size-fits-all benefits communication fails because your workforce isn't one-size-fits-all. Personalization increases relevance — and relevance drives action.
Tip 16: Segment Your Audience by Life Stage and Benefit Needs
Different employee groups have different priorities. Millennials and Gen Z prioritize non-traditional benefits like legal services and pet insurance, while Boomers and Gen X focus on traditional health coverage.
Create segments based on:
- Early career (20s-30s): Student loan assistance, mental health resources, telemedicine
- Parents: Dependent care, pediatric coverage, flexible scheduling
- Mid-career (40s-50s): Financial planning, college savings, eldercare resources
- Pre-retirement: 401(k) maximization, Medicare eligibility, retirement planning
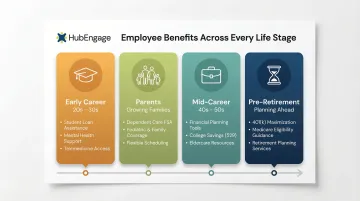
Targeted messaging for each segment reduces information overload and increases enrollment in the benefits that actually matter to each group.
Tip 17: Customize Communications by Location, Department, or Job Type
Benefits packages and communication needs often vary by location or role. A corporate office employee and a warehouse worker have different access points, reading habits, and benefit priorities.
Customization strategies:
- Highlight location-specific providers and facilities
- Emphasize benefits relevant to job type (physical therapy for manufacturing, mental health for high-stress roles)
- Adjust delivery channels based on work environment (SMS for frontline, email for desk-based)
- Translate materials for non-English speaking employee populations
Tip 18: Adapt Format and Tone for a Multigenerational Workforce
Your workforce may span Gen Z through Baby Boomers, each with different communication preferences. Gen Z and Millennials prefer short-form video, social media, and instant messaging, while Gen X and Boomers prefer email and in-person conversations.
Adaptation strategies:
- Offer the same information in multiple formats (video, infographic, detailed document)
- Use plain language that works across all age groups
- Provide both digital and print options when possible
- Balance visual, mobile-friendly content with comprehensive written resources
Tip 19: Train Managers to Be Benefits Communication Champions
Employees trust their direct managers 2.5 times more than CEOs to tell the truth about what's happening in their organization. This makes managers one of your most effective channels for benefits communication.
Equip managers with:
- Talking points for team meetings
- FAQs addressing common questions
- Ready-made messages they can forward
- Training on how to direct employees to resources
- Updates on benefit changes before they're announced company-wide
When managers communicate benefits in their own words, employees are far more likely to act on what they hear.
Tip 20: Provide Communications in Multiple Languages for Diverse Teams
With 22.3% of the U.S. population speaking a language other than English at home and 8.6% having limited English proficiency, English-only communications create serious barriers. For employees who aren't fluent in English, missing a benefits deadline or misunderstanding a plan isn't just inconvenient — it's costly.
Translation priorities:
- Open enrollment guides and plan summaries
- Deadline notifications and action-required messages
- Claims submission instructions
- Provider directories
- Wellness program materials
Even translating the highest-stakes documents — enrollment guides and deadline notices — closes a major comprehension gap for non-English-speaking employees.
Measure, Test, and Continuously Improve (Tips 21–25)
You can't improve what you don't measure. These tips help HR teams close the loop between communication effort and real outcomes.
Tip 21: Set Clear, Measurable Goals Before Each Campaign
Tie every benefits communication initiative to a specific measurable outcome so success can be evaluated objectively.
Example goals:
- Increase open enrollment completion rate from 85% to 95%
- Achieve 60% email open rate for benefits announcements
- Reduce HR help desk benefits inquiries by 30%
- Increase EAP utilization from 5% to 8%
- Drive 500 logins to benefits portal in first month
Without defined targets, you're left guessing whether your campaigns moved the needle at all.
Tip 22: A/B Test Subject Lines, Formats, and Send Times
Testing even simple elements can measurably lift open and click-through rates. Test one variable at a time and document results.
Elements to test:
- Email subject lines (benefit-focused vs. action-focused)
- Send times (morning vs. afternoon, weekday vs. weekend)
- Message length (brief vs. detailed)
- Visual vs. text-heavy formats
- Call-to-action wording
Over several cycles, even small gains—like a 10% lift in open rates—compound into significantly better overall reach.
Tip 23: Collect Employee Feedback Through Pulse Surveys
Send short, post-campaign or post-enrollment pulse surveys asking employees what was clear, what was confusing, and what they wish they'd known sooner.
Platforms like HubEngage allow HR teams to deploy quick surveys and capture real-time employee sentiment across channels—turning feedback into a continuous improvement loop. Keep surveys to 3-5 questions maximum to maximize completion rates.
Tip 24: Monitor Benefits Utilization Data to Find Communication Gaps
Low utilization of a specific benefit often signals a communication problem. For example, while 51% of employers offer Employee Assistance Programs, average utilization is only 5%, primarily due to lack of awareness.
Action steps:
- Partner with benefits providers to review quarterly utilization reports
- Identify benefits with enrollment below 10%
- Survey non-users to understand barriers
- Create targeted campaigns spotlighting underutilized benefits
- Track utilization changes after communication initiatives
Low utilization isn't always a sign employees don't want the benefit—often they simply don't know it exists or how to access it.
Tip 25: Treat Benefits Communication as an Ongoing Strategy, Not a One-Time Event
Effective benefits communication is a continuous program, not an annual checklist. Review your strategy quarterly, bring in employee input, and commit to iterating based on data rather than assumptions.
Quarterly review process:
- Analyze communication performance metrics
- Review benefits utilization trends
- Gather employee feedback
- Identify communication gaps
- Adjust calendar and messaging for next quarter
Teams that follow this cadence consistently report stronger enrollment numbers, higher utilization, and fewer repeat HR help desk inquiries over time.
Frequently Asked Questions
What is the best way to communicate employee benefits?
The most effective approach combines plain-language content, multi-channel delivery (email, SMS, mobile apps, digital signage), and a year-round communication calendar. Avoid relying solely on annual open enrollment pushes. Employees need consistent touchpoints throughout the year to understand and actually use their benefits.
What are the most effective employee benefits communications tools?
Effective tools include employee mobile apps, digital signage platforms, SMS messaging, intranet portals, and all-in-one platforms that centralize communications across channels. The best solution depends on your workforce: frontline workers need mobile-first tools, while desk-based employees may prefer email and intranet access.
What are the 5 C's of effective employee benefits communications?
The 5 C's framework includes: Clear (plain language), Consistent (year-round messaging), Customized (audience-segmented), Channel-appropriate (right medium for each group), and Continuous (ongoing feedback and improvement). This framework ensures benefits communications reach, engage, and inform all employees effectively.
How often should employers communicate about employee benefits?
Communicate at minimum monthly year-round, with higher frequency during open enrollment and life event moments. Brief, focused messages consistently outperform long annual blasts.
How do you measure the effectiveness of benefits communication?
Track email open and click-through rates, benefits enrollment rates, portal logins, HR help desk inquiry volume, and post-campaign pulse survey results. Compare utilization data before and after communication initiatives to measure real-world impact on employee behavior and benefit adoption.
How do you communicate benefits to frontline or deskless workers?
Frontline workers require non-email channels such as mobile apps, SMS, digital signage, and manager-led communication, since they rarely access a desktop or company email during their workday. Platforms built for deskless workforces deliver benefits content directly to employees' phones, ensuring equitable access regardless of work location.


