
Introduction
Employee benefits represent one of the largest non-payroll costs for employers—yet a staggering portion of that investment is wasted each year. According to WTW's 2025 research, while 84% of employees feel informed about their benefits, only 61% are actually satisfied with their offerings. That gap points to a communication and engagement problem, not a benefits design problem.
HR leaders face mounting pressure to justify benefits spend to finance teams, but ROI is nearly impossible to prove when employees aren't engaging with programs. The pain points are specific and costly: low enrollment rates, minimal utilization of wellness and mental health resources, and high benefits-related turnover.
The problem runs deepest among frontline and deskless workers, who make up over 80% of the workforce in industries like healthcare, retail, hospitality, and manufacturing — and who are routinely the hardest employees to reach with benefits information.
This article covers four actionable strategies any HR or communications leader can implement today: multi-channel communication that reaches every employee, data-driven gap analysis to identify underutilization, segmented personalization that delivers the right message to the right person, and year-round engagement that extends far beyond open enrollment.
TLDR
- Benefits ROI hinges on communication and engagement—not just the benefits package itself
- Close the awareness gap with multi-channel outreach—mobile, SMS, digital displays, and email—beyond the intranet alone
- Use engagement analytics to identify which benefits are underutilized, by which groups, and why
- Personalize benefits communication by role, life stage, and location so messages reach employees when they matter most
- Year-round touchpoints—not just open enrollment—keep benefits visible and relevant to employees
Why Most Employee Benefits Programs Fail to Deliver ROI
The core problem isn't the quality or range of benefits—most employers offer competitive packages. The breakdown happens at the awareness and access stage. Research shows that while 80% of workers at firms offering health benefits are eligible, only 61% actually enroll. In retail, the coverage rate drops to just 34%.
Low benefits engagement creates real business costs HR leaders can quantify:
- Higher voluntary turnover - Employees who don't value their benefits are more likely to leave for competitors
- Increased absenteeism - Employees miss an average of 6.1 days of work due to health-related issues when preventive health programs go unused
- Productivity drag - 56% of employees are "job hugging"—staying out of necessity rather than satisfaction—and these workers are 54% less likely to be holistically healthy
The gap runs deepest for frontline, deskless, and distributed workers who rarely check email and are systematically left out of standard benefits communications. When 69% of organizations prioritize email but 54% of deskless workers have limited email access, benefits spending quietly leaks ROI at scale—before it ever reaches the employees who need it most.
Way 1: Communicate Benefits Through Every Channel Your Employees Actually Use
The Awareness Barrier
Awareness is the first and most critical barrier to benefits ROI. If employees don't know a benefit exists, it won't be used. Period. Organizations typically default to email-only or intranet-only communications, which structurally excludes frontline and shift workers and drives low utilization rates across the board.
Only 1% of communicators feel very effective at reaching frontline workers. Meanwhile, one in four workers say they don't know where to find critical information. For a benefits strategy, that's not a communication problem — it's a utilization problem with a direct cost.
Build a True Multi-Channel Strategy
A multi-channel benefits communication strategy means reaching employees through:
- Mobile push notifications - Delivered directly to phones for time-sensitive updates
- SMS text alerts - 90-98% open rates compared to email's 20-30%
- Digital display screens - In breakrooms and common areas where frontline workers gather
- Email - Still effective for detailed, long-form content for desk workers
- Intranet/web portals - Central hub for comprehensive benefits information
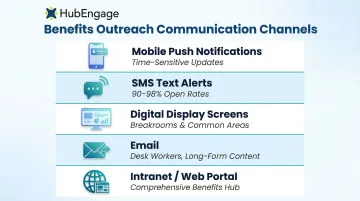
The goal is to meet employees where they already are, not make them come to you. This approach is especially critical during open enrollment windows when time-sensitivity matters. 77% of employees plan to spend more time reviewing benefit elections this year due to inflation concerns—but only if they receive the information through accessible channels.
Eliminate Manual Multi-Channel Effort
Platforms like HubEngage let HR teams publish one benefits message that auto-formats across mobile apps, web, email, SMS, and digital signage simultaneously. No separate drafts per channel, no version inconsistencies — just full workforce reach from a single send.
Once distribution is handled, the next question is whether employees are actually absorbing the information.
Use Pulse Surveys to Diagnose the Problem
Pulse surveys delivered via push notification or SMS serve as a quick litmus test for benefits awareness. Are employees not engaging because they don't know about a benefit, or because they don't understand how to use it? This distinction matters—an awareness problem requires broader communication reach, while an education problem requires clearer instructions and support resources.
Optimize Through A/B Testing
A/B testing communications—different subject lines, message formats, timing, or channels—allows HR teams to use live performance data to optimize future benefits messaging. Track open rates, click-throughs, and enrollment completions by variant to identify what actually drives action, then standardize what works.
Way 2: Use Engagement Data to Find and Fix Benefits Utilization Gaps
Move Beyond Enrollment Numbers
Benefits engagement analytics show HR leaders not just who enrolled, but which benefits are actively being used, which are underutilized, and where the biggest gaps exist by department, location, tenure, or role. This contrasts sharply with the "set and forget" model where HR reports enrollment numbers but has no visibility into actual utilization or value delivered.
Conduct a Data-Informed Benefits Audit
A practical benefits audit overlays enrollment data with demographic or workforce data to surface patterns:
- Employees at a certain location never using mental health EAP resources
- Parents not using emergency childcare benefits despite enrollment
- Frontline workers unaware of financial wellness tools
- High-deductible plan enrollees avoiding preventive care due to out-of-pocket cost concerns (50% of employees report this barrier)

This segmented view tells HR exactly where to intervene — and with which employee groups — instead of launching one-size-fits-all awareness campaigns.
Validate Data with Surveys
Survey data can validate or challenge utilization data. If utilization of a wellbeing benefit is low, a short survey might reveal employees don't understand how to access it — pointing to a communication fix rather than a benefits redesign. This distinction saves money and improves outcomes.
Take EAP programs as a concrete example: average utilization sits at just 5%, yet companies that actively promote their EAPs see up to 3x higher usage. In most cases, the benefit isn't the problem — the communication is.
Build a Credible ROI Story
Once you've identified the gaps and confirmed the root causes, that data becomes your internal ROI case for leadership and finance. Translate underutilized benefits into avoided costs:
- Preventive health programs → reduced absenteeism and lower healthcare claims
- Financial wellness tools → reduced financial stress and improved productivity
- Mental health resources → lower stress-driven turnover
The numbers back this up: employers expect a $2.30 return for every $1 invested in employee health — but that return only materializes when employees actually use the programs. Closing utilization gaps is where the ROI is won or lost.
Benchmark for Context
Benchmark utilization trends against your own historical data and relevant industry norms. Is EAP usage climbing quarter over quarter? Are specific departments still lagging? These comparisons give leadership concrete evidence of progress — and a defensible rationale for where to invest next in benefits communication.
Way 3: Personalize Benefits Communication for Different Employee Segments
Why One-Size-Fits-All Fails
A one-size-fits-all benefits communication approach fails in a multigenerational, multi-role workforce. A 24-year-old warehouse associate has different benefits priorities than a 45-year-old manager approaching retirement or a new parent in a customer service role. When employees receive irrelevant benefits messaging, they disengage—and engagement with all future communications drops.
78% of employees say benefits personalization is more important than benefits integration. This isn't a nice-to-have—it's what employees expect.
Key Segmentation Dimensions
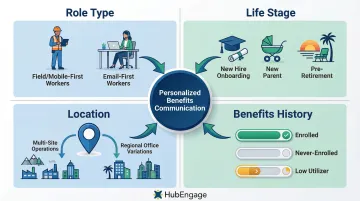
HR and communications leaders should segment by:
Role Type:
- Frontline vs. desk workers have different access patterns and communication preferences
- Shift workers need mobile-first communications, not email-dependent processes
Life Stage:
- New hires need comprehensive benefits orientation
- New parents need childcare and parental leave information
- Employees approaching retirement need 401(k) and healthcare transition guidance
Location:
- Multi-site employers need location-specific benefits information
- Regional variations in healthcare networks or local wellness programs require targeted messaging
Benefits History:
- Recently enrolled employees need usage education
- Never-enrolled employees need awareness and enrollment support
- Enrolled but low utilizers need engagement and activation campaigns
Trigger Communications at Life Events
Segmentation tells you who to reach — life events tell you when. Life events are the moments when benefits shift from abstract to urgent — and employees are actively looking for guidance. Targeted benefits education at these touchpoints consistently improves both utilization rates and employees' sense that their employer genuinely supports them.
Common high-value trigger moments include:
- Marriage or domestic partnership — health coverage additions, beneficiary updates
- New child — parental leave, dependent care FSA, childcare benefits
- Health diagnosis — EAP resources, disability coverage, specialist networks
- Job change or promotion — benefits tier adjustments, new eligibility windows
Proactive outreach at these moments — not a static portal — is what drives action.
Maximize the Onboarding Window
The onboarding window is one of the highest-leverage moments for benefits communication. New employees are most receptive to learning about their benefits package, yet many rarely go beyond a compliance-driven enrollment checklist.
A personalized, phased onboarding sequence improves first-year retention and benefits utilization from day one. Instead of overwhelming new hires with everything at once, deliver benefits information in digestible phases aligned with their first 90 days.
Way 4: Build Year-Round Benefits Engagement, Not Just Open Enrollment Campaigns
The Open Enrollment Trap
The vast majority of benefits communication is concentrated in a two-to-four-week annual window, leaving employees with no reinforcement or reminders for the remaining 48-plus weeks of the year. Benefits that aren't top-of-mind don't get used, and employees who feel their employer doesn't communicate consistently about benefits are more likely to undervalue their total compensation package.
65% of employees are open to receiving information from their employer outside of open enrollment to help them better understand their benefits. They want year-round engagement—so why aren't we providing it?
Practical Year-Round Tactics
Maintain year-round benefits engagement through:
Seasonal Reminders:
- Mental health resources in January (New Year stress and goal-setting)
- FSA spend reminders in November (use-it-or-lose-it deadlines)
- Preventive care reminders in Q1 (annual physicals and deductible resets)
- Summer wellness challenges tied to health benefits
Awareness Month Tie-Ins:
- Mental Health Awareness Month (May)
- Heart Health Month (February)
- Financial Literacy Month (April)
- Open Enrollment Preparation (September/October)
Wellness Challenges:
- Connect health benefits to participation and community
- Step challenges, hydration goals, or meditation streaks
- Tie completion to recognition or small rewards
These touchpoints don't require major effort. A reliable, lightweight communication infrastructure is all it takes to make consistent outreach practical.
Leverage Gamification for Ongoing Participation
Point systems, challenges, and recognition tied to benefits participation turn passive benefit holders into active ones. Year-round gamification keeps employees connected to their benefits long after open enrollment closes:
- Completing a wellness assessment
- Attending a financial wellness webinar
- Using a preventive care benefit
- Engaging with mental health resources
- Participating in benefits education sessions
HubEngage applies gamification across communications, recognition, and engagement activities, making it practical for HR teams to build this kind of participation culture without manual overhead.
Employees earn points for viewing content, acknowledging messages, taking surveys, and recognizing peers. Those points can be redeemed through leaderboards, gift cards, and rewards — giving employees a concrete reason to stay engaged all year.
Frequently Asked Questions
What are the top 3 most sought after employee benefits?
Health insurance, retirement savings plans (401k), and paid time off consistently top the list. However, the perceived value of these benefits is heavily influenced by how well they're communicated and how easy they are to access.
What does a 20% ROI mean?
In employee benefits, a 20% ROI means every dollar spent on benefits programs and communications returns $1.20 in measurable value. That return shows up as improved retention, reduced absenteeism, higher productivity, and lower healthcare costs.
How do you measure ROI on employee benefits?
Measure ROI through key outcomes: turnover rate changes, absenteeism rates, healthcare cost trends, benefits utilization rates, and employee satisfaction scores. Compare these metrics against the total investment in the benefits program to calculate net return.
Why do employees not use their benefits?
The primary reasons are lack of awareness, confusion about how to access or use a benefit, perception that a benefit doesn't apply to them, and difficulty accessing information—especially for frontline or non-desk workers who are often excluded from standard email-based communications.
How does employee communication affect benefits utilization?
Employees cannot engage with benefits they don't know about, don't understand, or can't easily access. Organizations with proactive, multi-channel communication strategies consistently see higher utilization rates and stronger overall benefits satisfaction.
How often should companies communicate about employee benefits?
Move beyond annual open enrollment toward a year-round cadence: monthly benefits spotlights, life event-triggered messages, and onboarding communications that keep benefits visible and relevant when employees need them most.


